By Bryan Markinson, DPM
Educational podiatric pathology case review series
Patient: 68-year-old female
Lesion Locations: Right third toe (lateral skin) and right hallux nail bed
Clinical Presentation: Granulating lesion on the lateral third toe of one to two years duration (patient thought it was a blister), and a non-healing, oozing wound on the right hallux nail bed following self-trimming of a thickened, discolored nail. Prior history of squamous cell carcinoma (SCC) and basal cell carcinoma (BCC) at other sites.
A 68-year-old female with a history of multiple cutaneous malignancies was referred for definitive care of a malignant eccrine porocarcinoma of the right third toe, confirmed on prior biopsy by the referring podiatrist. At initial presentation, she also had a non-healing wound on the right hallux nail bed — the result of self-trimming a chronically thickened, detached nail — which had never healed and continued to ooze. Workup for the porocarcinoma included PET/CT (negative for distant metastasis), oncology consultation, and sentinel lymph node (SLN) biopsy planning. Three weeks later, on the day of scheduled surgery, the hallux wound remained unhealed and a nail bed punch biopsy was added to the operative plan.
Take a moment to review the clinical images below to see how Dr. Markinson arrived at these diagnoses.
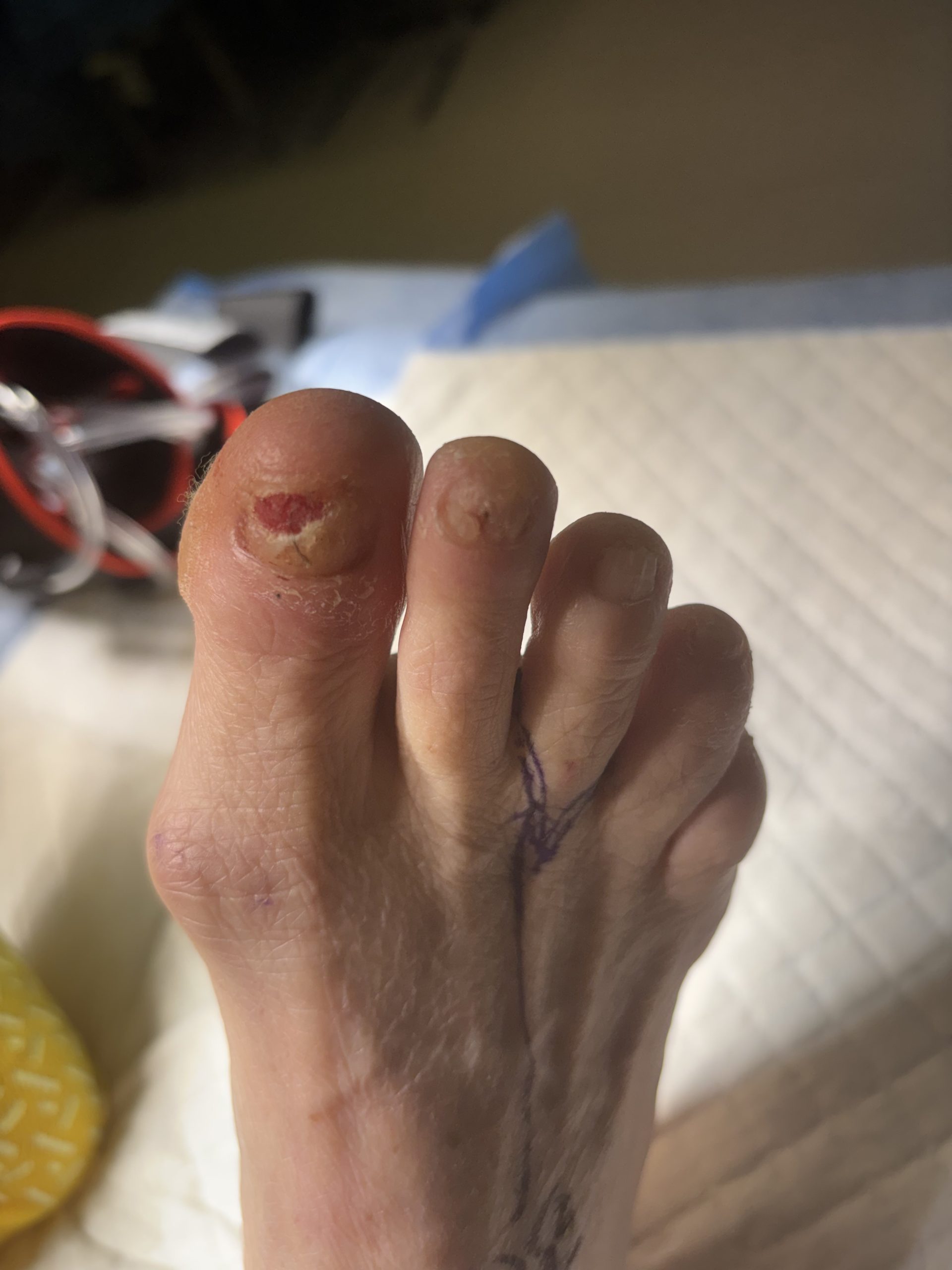
(Clinical photograph: pre-oped delineating amputation incision and right hallux nail bed lesion, right foot)
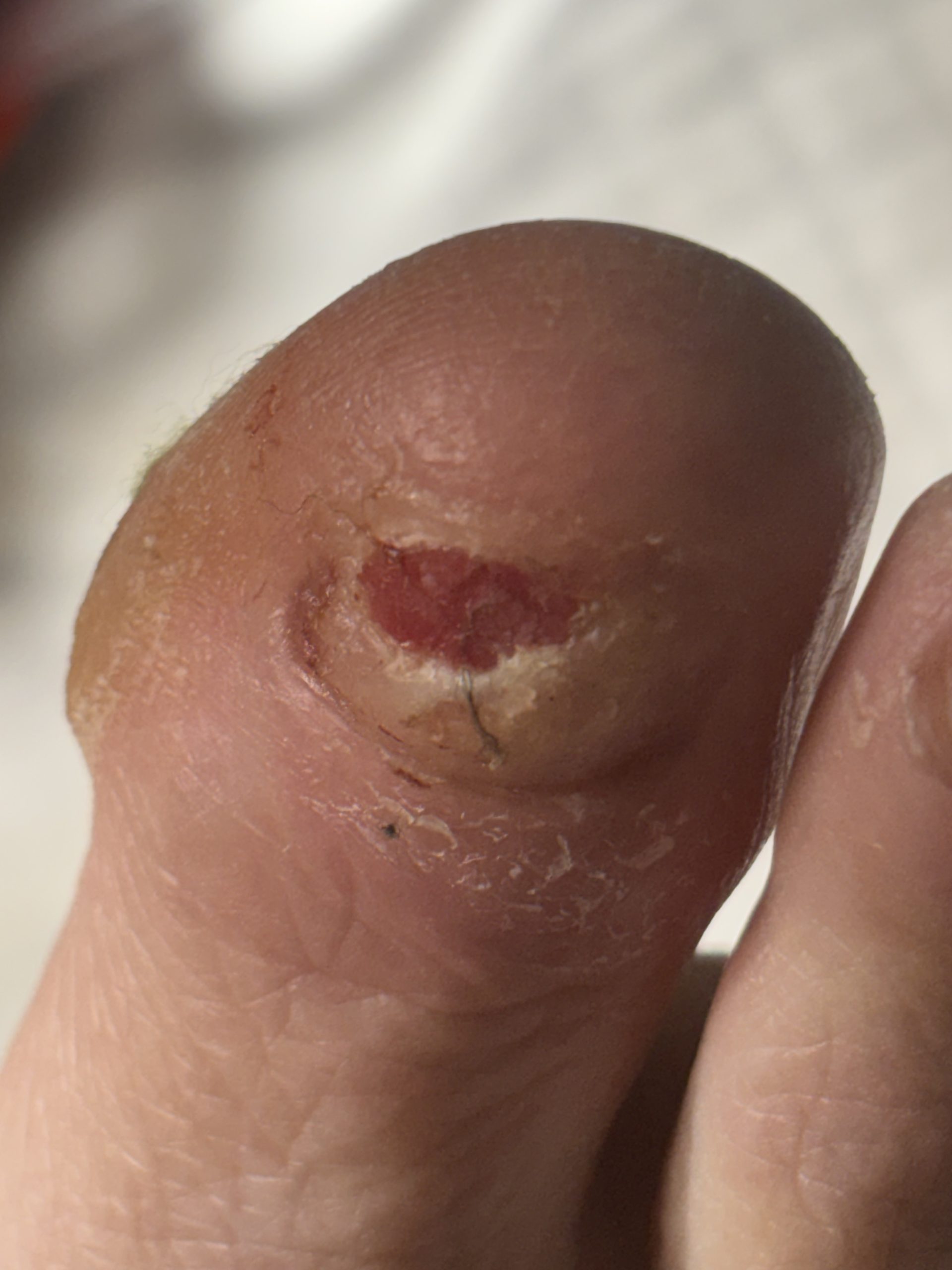
(Clinical photograph: non-healing wound, right hallux nail bed)
Four specimens were submitted at the time of surgery:
Specimen A — Porocarcinoma, Third Toe
Histologic examination of the amputated third digit confirmed:
Specimen B — Basal Cell Carcinoma, Nail Bed
The nail bed punch biopsy revealed:
Specimens C & D — Sentinel Lymph Nodes
When evaluating non-healing or granulating lesions of the nail unit and digit, several diagnoses must be considered. The three most important mimickers are outlined below.
Etiology: Malignant transformation of subungual melanocytes; accounts for a disproportionate share of melanoma in darker-skinned populations
Histology:
Key Distinction: Subungual melanoma typically presents with longitudinal melanonychia and demonstrates pagetoid spread on histology — neither of which is a feature of nail bed BCC. Immunohistochemistry (S-100, SOX10, Melan-A) can confirm melanocytic process.
Etiology: Most common malignant tumor of the nail unit; frequently HPV-associated (types 16/18) in this location
Histology:
Key Distinction: Subungual SCC is the most common nail unit malignancy and shows squamous differentiation with keratin production. HPV in-situ hybridization or p16 immunostaining can help support an HPV-driven etiology.
Etiology: Reactive vascular proliferation, often following minor trauma or nail manipulation; also mimics malignancy clinically
Histology:
Key Distinction: Pyogenic granuloma and chronic granulation tissue are the most common benign mimickers of nail unit malignancy following trauma — exactly the scenario in this case, where the patient attributed the wound to nail trimming. The absence of cytologic atypia, malignant architecture, and the lobular vascular pattern distinguish these reactive lesions from carcinoma. When healing fails to progress with standard care, biopsy is essential.
Porocarcinoma is a rare malignancy of eccrine sweat gland origin characterized by ductal and poroid differentiation, elevated mitotic activity, and meaningful metastatic potential. Nail bed BCC — while histologically identical to BCC elsewhere — is exceptionally rare in the toe, making this a coincidental dual occurrence in the same foot. Both diagnoses were confirmed in the setting of negative sentinel lymph nodes, supporting localized disease at the time of excision.
Key Takeaways:
| Feature | Porocarcinoma | Nail Bed BCC | Subungual Melanoma | Subungual SCC |
| Origin | Eccrine sweat glands | Basal cell layer | Melanocytes | Squamous epithelium |
| Nail unit occurrence | ❌ Rare | ❌ Extremely rare | ✅ Classic site | ✅ Common but likely underestimated due to misdiagnosis |
| Metastatic potential | ✅ Yes | ❌ Rare | ✅ High | ✅ Moderate to low |
| Key histologic clue | Ductal/poroid cells, high mitoses | Peripheral palisading, retraction artifact | Malignant melanocytes | Keratin pearls, dyskeratosis |
| Longitudinal melanonychia | ❌ No | ⚠️ Sometimes | ✅ 30% of cases preceded by longitudinal melanonychia | ❌ No |
| Behavior | Aggressive | Locally aggressive | Slow growing | Locally aggressive |
Synchronous rare malignancies in the same foot (porocarcinoma of the toe and BCC of the nail bed) serve as a powerful reminder that any non-healing lesion demands histologic confirmation. When the clinical story doesn’t add up, the microscope tells the truth.
Sagis Podiatric Pathology is proud to support dermatology residents and dermatology residency programs through high-quality educational content and learning resources.
Follow us on Instagram for more micro-learning opportunities with interactive cases and podiatric pathology insights.
Related Case Reviews
Join Our Dermpath Educational Community
Access expert-led content, and stay in the loop on upcoming sessions and resources from our Dermpath Educational community.
Did you know we are diagnostics lab?
Sagis Podiatry delivers accurate, timely diagnoses with dedicated support from our lab team and direct access to our pathologists.