By Dr. Vickers, Sagis Diagnostics
Educational dermpath case series for dermatology residents
Patient: 17-year-old male
Lesion Location: Diffuse hypopigmented patches across the body
This biopsy is from a 17-year-old male patient with white patches present for 2 years at the time of biopsy. Take a moment to review the clinical and histologic images below, do you know how Dr. Vickers came to this diagnosis?
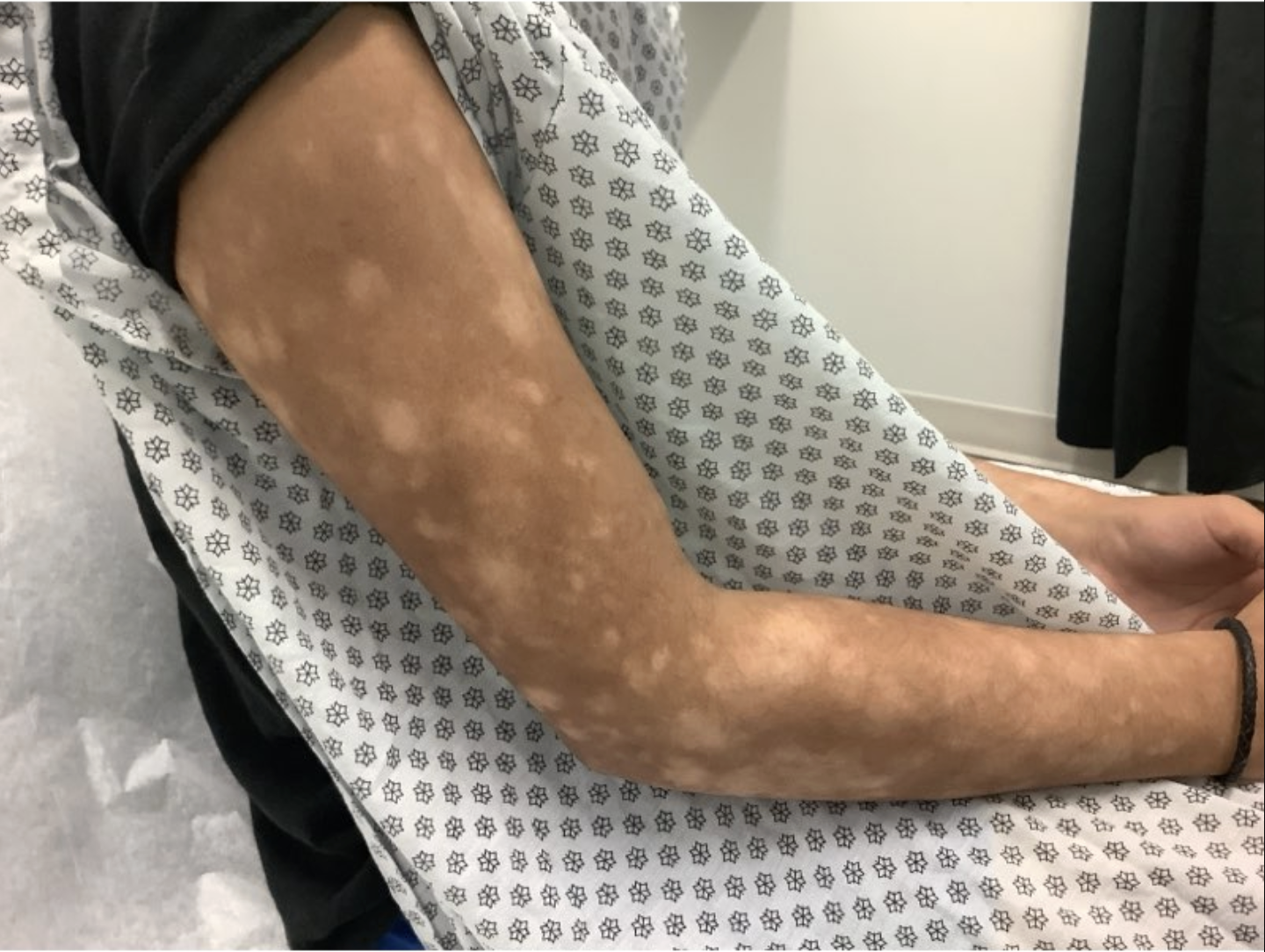
(Image 1: Clinical photo — hypopigmented patches on patient’s skin)
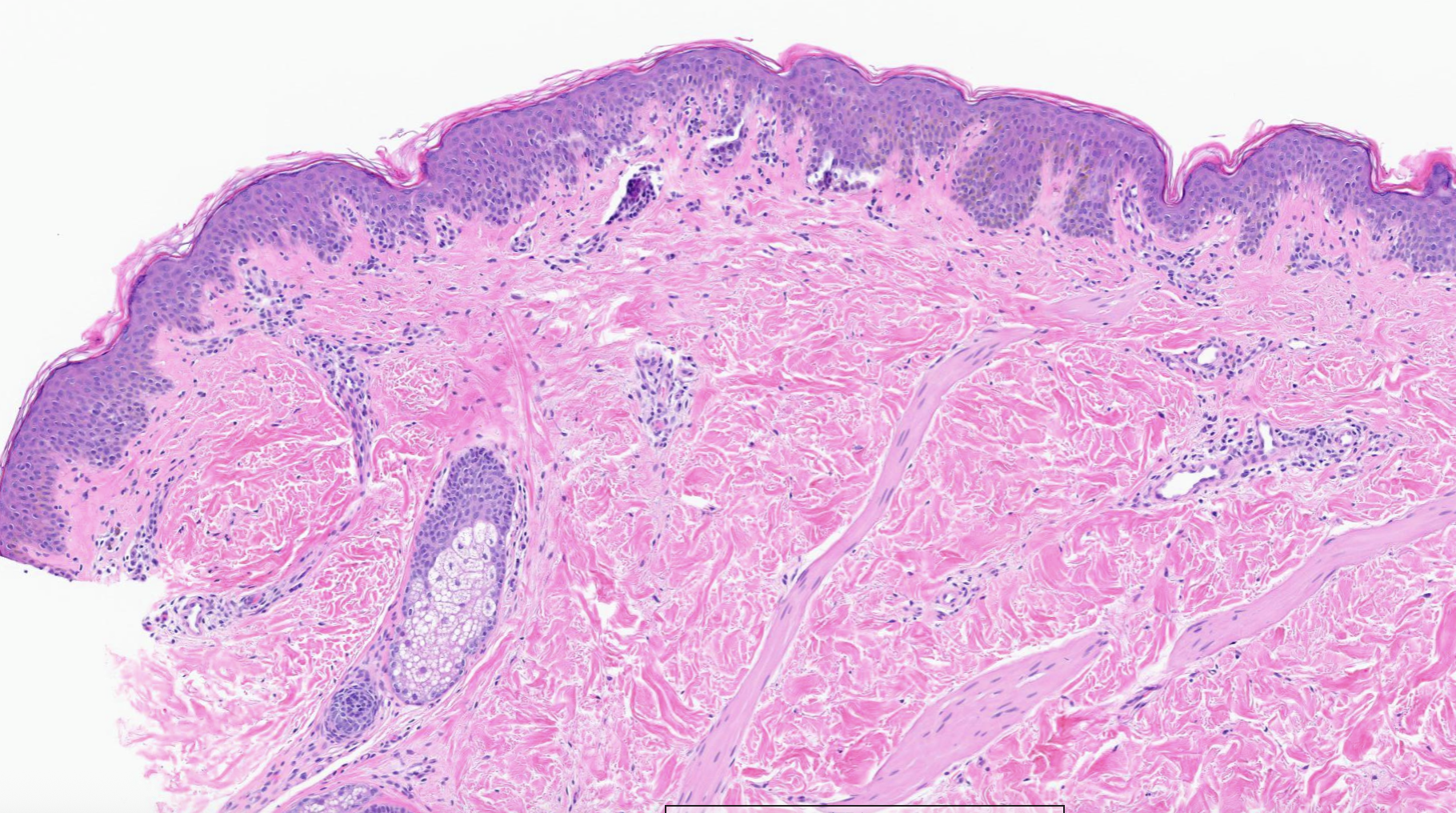
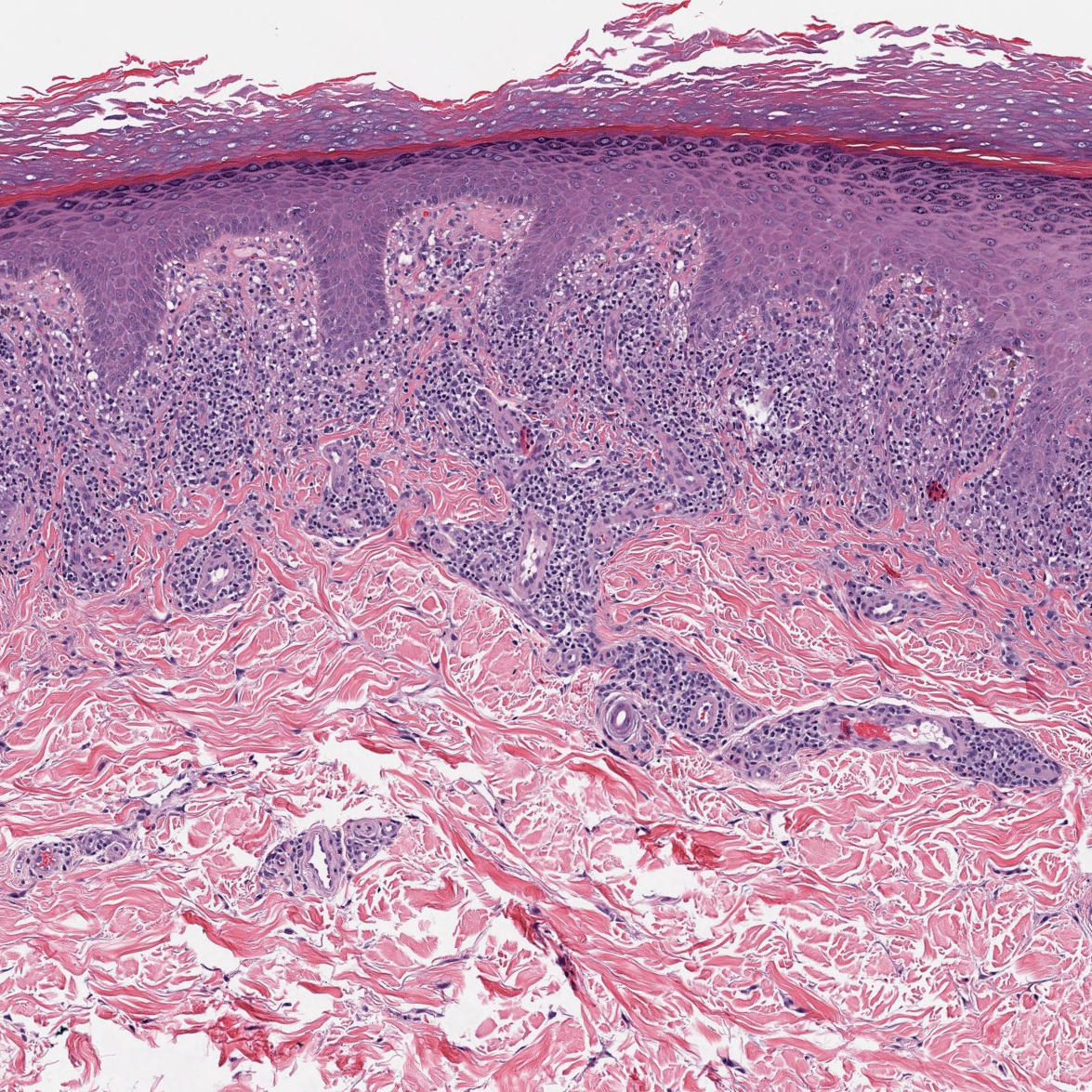
(Image 2: High power showing atypical lymphocytes with perinuclear halos)
Key Histologic Findings
On examination, several defining features stand out:
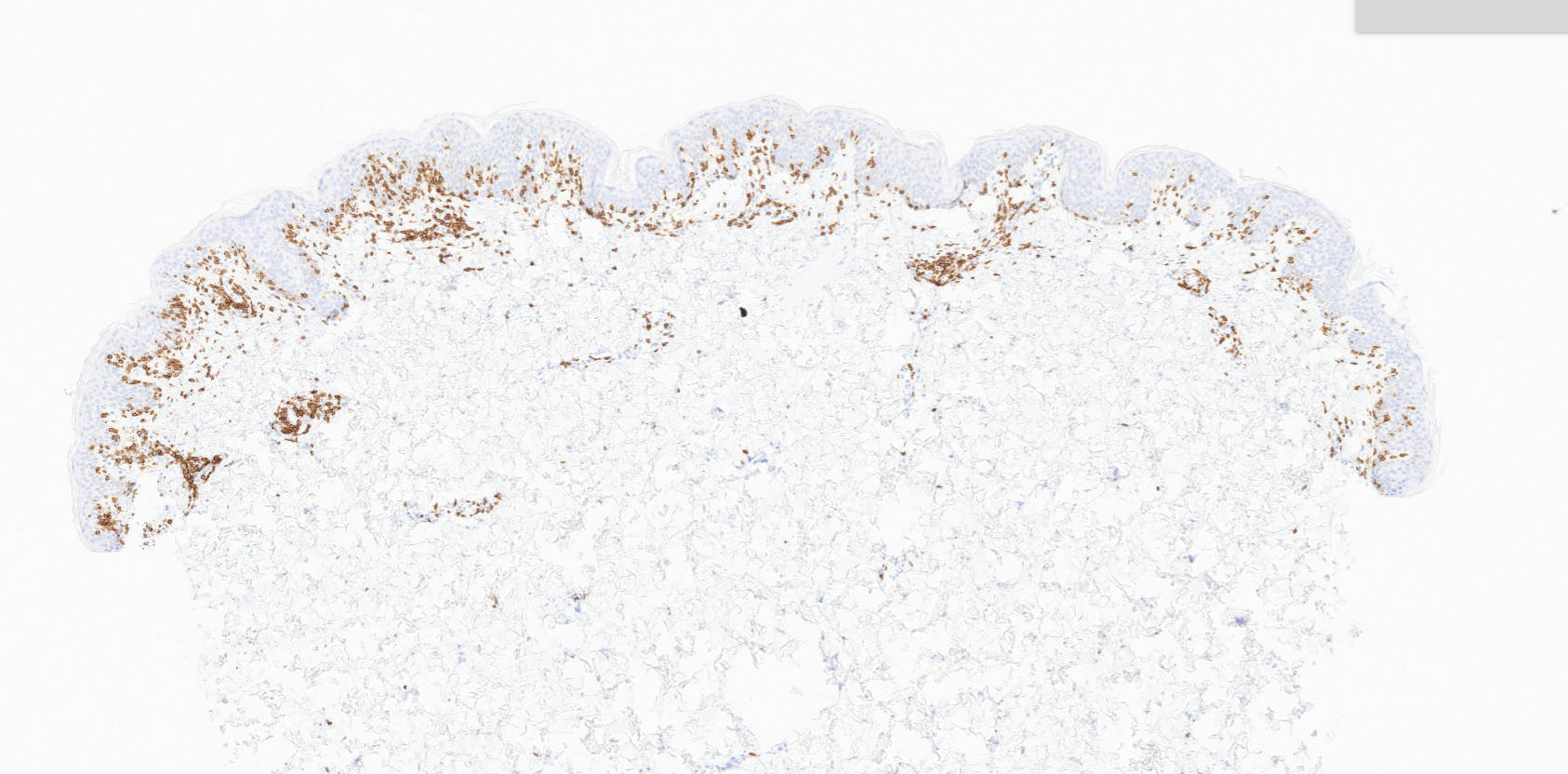
(Image 3: IHC CD3 – Medium power showing epidermotropism)
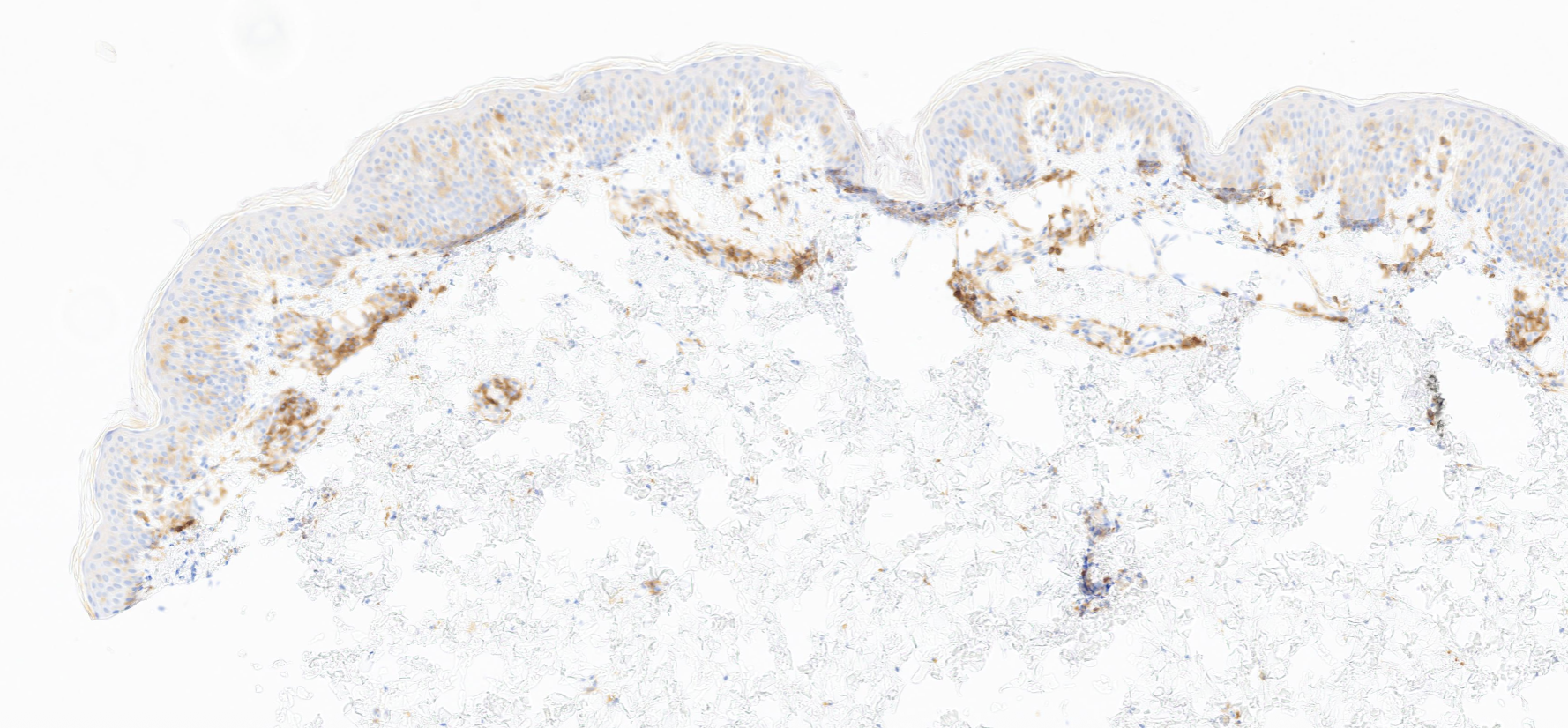
(Image 4: CD4)
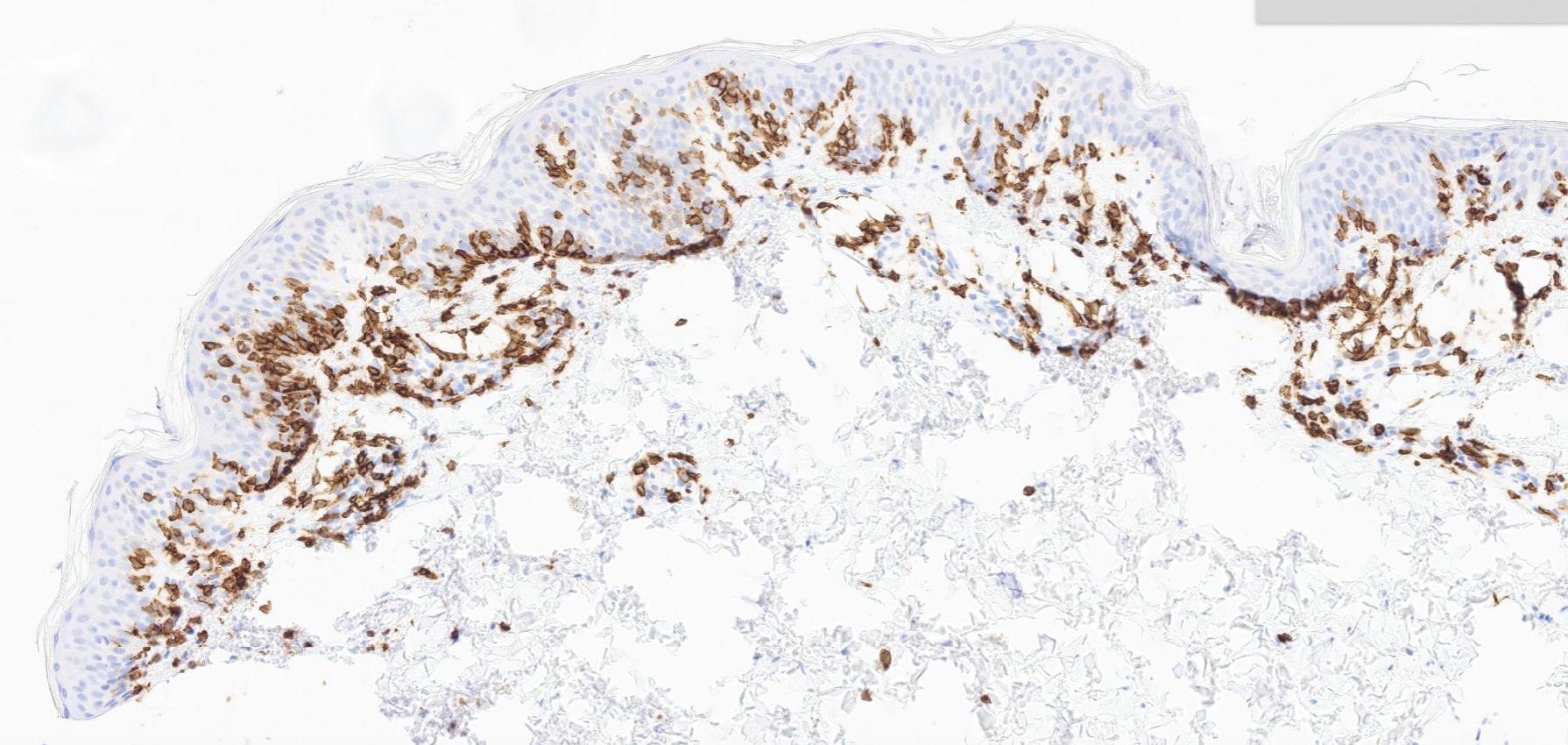
(Image 5: IHC CD8)
Differential Diagnosis: Three Common Mimickers
When evaluating hypopigmented patches in a young patient, several differentials come to mind. Let’s walk through the three most likely contenders and highlight what sets them apart.
Etiology: T-cell mediated lichenoid interface dermatitis; may be idiopathic, drug-induced, or autoimmune
Histology:
Key Distinction: Lichen planus produces a band-like infiltrate at the DEJ with Civatte bodies, but the lymphocytes are mature and polyclonal. CD8+ MF displays nuclear irregularity and epidermotropism with halos — features absent in LP. Immunostains demonstrating a clonal CD8+ T-cell population and TCR gene rearrangement studies confirm MF.
(Image 6: Lichen planus — band-like infiltrate and saw-tooth rete ridges for comparison)
Etiology: Epidermal barrier dysfunction with type 2 immune hypersensitivity; often atopic in origin
Histology:
Key Distinction: Eczema and CD8+ MF can appear deceptively similar at low power, both showing a superficial lymphocytic infiltrate. However, spongiotic dermatitis features spongiosis and lacks the atypical lymphocytes and halo-forming epidermotropism of MF. The absence of T-cell clonality on TCR gene rearrangement studies further supports eczema over MF.
Etiology: Type IV delayed hypersensitivity reaction to a systemically administered medication
Histology:
Key Distinction: Drug eruptions may show interface changes superficially overlapping with patch-stage MF, but the lymphocytes are reactive rather than clonal. Prominent eosinophils and a temporal relationship with a medication favor drug eruption. Drug eruptions resolve with drug withdrawal; CD8+ MF is a T-cell lymphoma requiring ongoing management.
The presence of epidermotropism, atypical lymphocytes with perinuclear halos, and a dominant CD8+ T-cell immunophenotype is diagnostic. This variant is not associated with the typical CD4+ phenotype, setting it apart from conventional MF. Correct identification matters: these patients are often young, and an accurate diagnosis directs appropriate therapy while sparing unnecessary workup for other conditions.
Key Takeaways for Residents:
| Feature | CD8+ Hypo MF | Lichen Planus | Eczema | Drug Eruption |
| Patient profile | Kids, teens, melanated skin | Any age | Any age, atopic | Any age |
| Atypical lymphocytes | ✅ Present | ❌ Absent | ❌ Absent | ❌ Absent |
| Epidermotropism w/ halos | ✅ Present | ❌ Absent | ❌ Absent | ❌ Absent |
| Eosinophils | ❌ Absent | ❌ Rare | ✅ Possible | ✅ Common |
| Spongiosis | ❌ Absent | ❌ Absent | ✅ Present | ✅ Possible |
| CD8+ phenotype | ✅ Dominant | ❌ Mixed | ❌ Mixed | ❌ Mixed |
| T-cell clonality | ✅ Yes | ❌ No | ❌ No | ❌ No |
| Hypopigmentation | ✅ Characteristic | ❌ Not typical | ❌ Not typical | ❌ Not typical |
| Behavior | Indolent MF | Benign / chronic | Benign / chronic | Resolves w/ drug removal |
💬 Final Thought
CD8+ Hypopigmented Mycosis Fungoides is a classic dermatopathology “look-alike” that rewards careful microscopic examination. Remember: the “halos” tell the story.
Sagis Diagnostics is proud to support dermatology residents and dermatology residency programs through high-quality educational content and histopathologic learning resources.
Follow us on Instagram for more micro-learning opportunities with interactive cases and pathology insights.
Are you interested in viewing other dermpath diagnostic videos like this?
Type a diagnosis in the search window below to see applicable videos.
Related Case Reviews
Join Our Dermpath Educational Community
Access expert-led content, and stay in the loop on upcoming sessions and resources from our Dermpath Educational community.
There are no specimen slides available for this interview session. Enjoy the session!
Did you know we are diagnostics lab?
Sagis Dermatopathology delivers accurate, timely diagnoses with dedicated support from our lab team and direct access to our dermatopathologists.
CAREER RESOURCES
Looking for a Job after Graduation?
Click: https://www.sagisdx.com/post-residency-fellowship/
Let us know what you’re looking to specialize in. We’ll help connect you to our wide network.